For the 170,000 children born every year with a cleft palate, their future can rest on one simple question. Were they born in a developed country with plenty of doctors and resources waiting to help them fix their deformity, or were they born in an impoverished country with few doctors, fewer resources and an average income of just a few dollars a day?
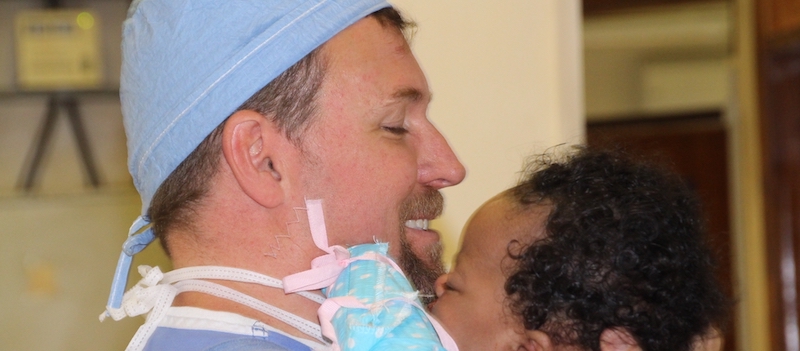
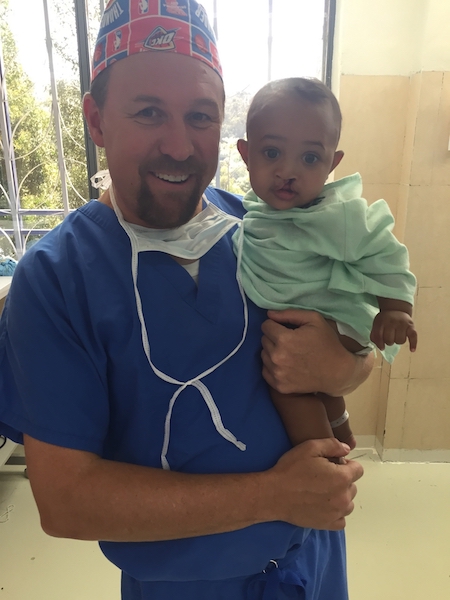
Our own Dr. Robert Glade is working to even the playing field. In September 2016, Dr. Glade flew to Addis Ababa, Ethiopia with the Free to Smile Foundation to help children in need. Freedom to Smile (FTS) works to raise awareness about cleft palate and dental issues, implement training programs for local doctors and offer surgical assistance to needy children worldwide.
What Is Cleft Palate or Cleft Lip?
Cleft palate and cleft lip are two very similar conditions that both occur when a child is still forming in the mother’s womb. With cleft palate, the roof of the mouth and upper lip never close completely. With cleft lip, the upper lip alone never closes completely. It can be cleft on one or two sides.
A cleft palate is more than just a physical defect. Children with clefts can feel isolated and may be actively shunned by their communities. Even mild clefts can cause speech impediments, making it even more difficult to find acceptance within communities. Severe clefts can even make eating difficult, especially for young children.
How Is It Fixed?
A cleft palate can be fixed as early as 9 to 12 weeks. The child is put under general anesthesia, and the surgeon connects all necessary muscles. Tissues are neatly sewn together to create a natural upper lip shape. Follow-up surgeries may be necessary to shore up bone structure, fix breathing or speaking issues during development or to make other adjustments.
Fixing the physical aspects is only the first step. In some communities, clefts are seen as a sign of bad karma, the mark of evil spirits or a similar ill omen. FTS is sensitive to cultural needs and helps children integrate into their communities after surgery. FTS also works to break the stigma surrounding the condition while honoring tradition and customs.
Solutions Within Reach
Most families in impoverished countries could never afford corrective surgery on their own. The magic starts happening with volunteers. Volunteer doctors, like Dr. Glade, and staff bring the basic surgical costs down to as little as $275. That’s all it takes to change the rest of a child’s life for the better. Monetary support comes from individual donations, employer matching programs and retail charity initiatives like Amazon Smile.
FTS doesn’t just want to ride in, perform a few surgeries and ride off into the sunset. Through comprehensive education and training programs for local surgeons, they hope to make communities self-sufficient. FTS can then bring their hands-on initiatives to a new community.
September in Addis Ababa
On September 26th, 2016, a small FTS surgical team arrived at CURE Pediatric Hospital in Addis Ababa, Ethiopia. With its bright green and yellows, CURE Hospital is a cheery beacon of hope for the 30 children and their families that have traveled to meet the surgical team. CURE Hospital is supported by a nonprofit and was founded primarily to serve children in the region born with physical abnormalities, like cleft palate and clubfoot.
Dr. Glade, who has previously volunteered his time in China, was one of two oral surgeons on the crew. Over the course of four days, the surgical team completed 23 surgeries on babies under the age of 1 year, 7 surgeries on children between 1 and 5 and one final surgery on a 44-year-old man!
A Day in Addis Ababa
Running each day like a well-oiled machine is the key to fitting numerous surgeries in just a few days.
Take a look at the average surgery schedule:
- 7:30 AM: While the surgeons check on yesterday’s patients, a nurse starts moving today’s patients through pre-op procedures
- 8:00 AM: Surgeries begin. Each could take 1 to 6 hours.
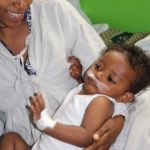
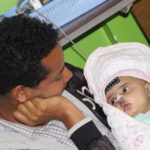
- Post-Operations: Patients are taken right to the post-anesthesia care unit, or PACU. Once they’re awake enough to be hungry, babies are given to their mothers to breastfeed right away.
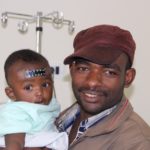
- Post-“Lunch”: Patients are moved into a “family ward” where their fathers can dote on them and spend time with both mother and baby
- Overnight: Patients are monitored carefully
- Late Next Morning: After the parents get the final instructions and bandages are changed, the patients are ready to go home!
Ethiopia is just one of many countries in need of programs like FTS to get help to children in need. Wherever the road may take him, Dr. Glade is looking forward to his next trip.